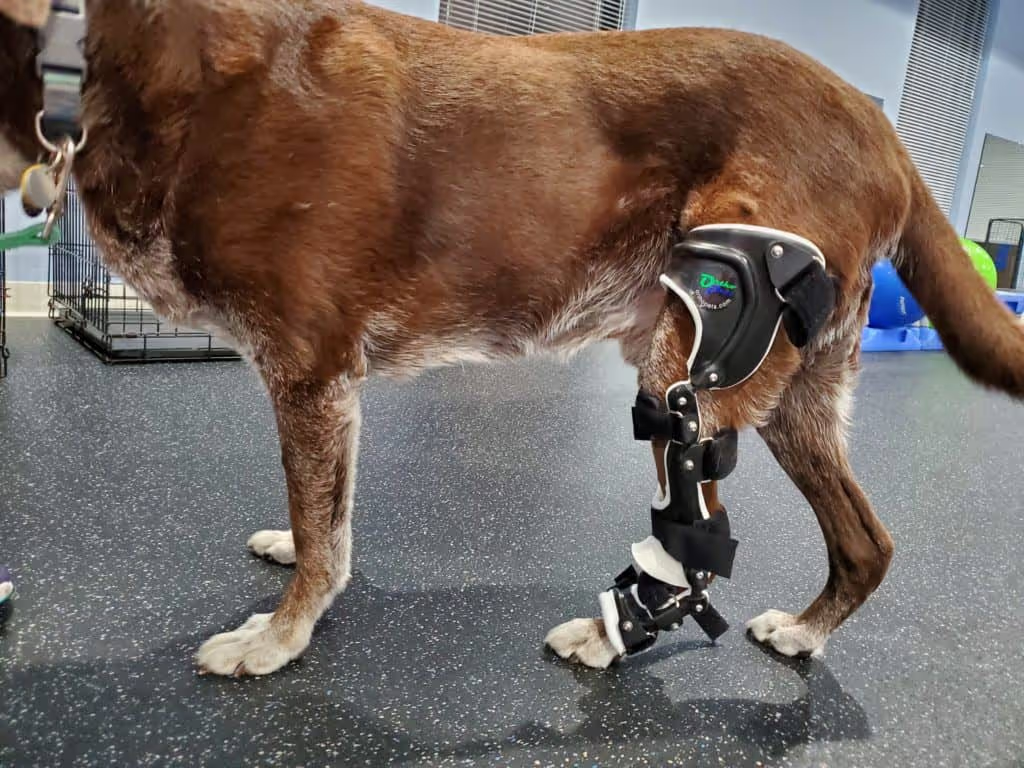
Fiberglass Impression versus Digital Limb Scanning in VOP

By Bobbie Adams, RVT, CCRP, MSPO, LPO
Impression (noun) – an impression is taken of the affected limb to replicate it for fabrication purposes.
The Veterinarians at OrthoPets Partner Clinics and VOP Certified Prosthetist Orthotists (CPOs) use a material called Fiberglass to take an impression of the affected limb. After the fiberglass impression is created, the impression is either mailed to OrthoPets, where a VOP Modifier scans the impression with a 3D scanner for fabrication via CAD/CAM (computer aided design / computer aided manufacturing). Or for faster case processing, the impression can be scanned with 3D scanner and sent digitally to the OrthoPets laboratory for fabrication via CAD/CAM (computer aided design / computer aided manufacturing).
But why? – why do we use a Fiberglass impression to capture limb shape over new technologies such as digital limb scanning? Let’s dig in, but first – some history.
History of hand casting1
Hand casting with Plaster of Paris (POP) is a casting technique dating back to the 1850s when used for bandaging and immobilization of human limbs. More recent historical uses in the human orthotic and prosthetic (O&P) field include:
• Sarmiento humeral fracture casting
• Hip spica casting for pediatric developmental hip dysplasia
• Ponseti serial casting for pediatric clubfoot
• Scoliosis management
• Post-amputation rigid dressings
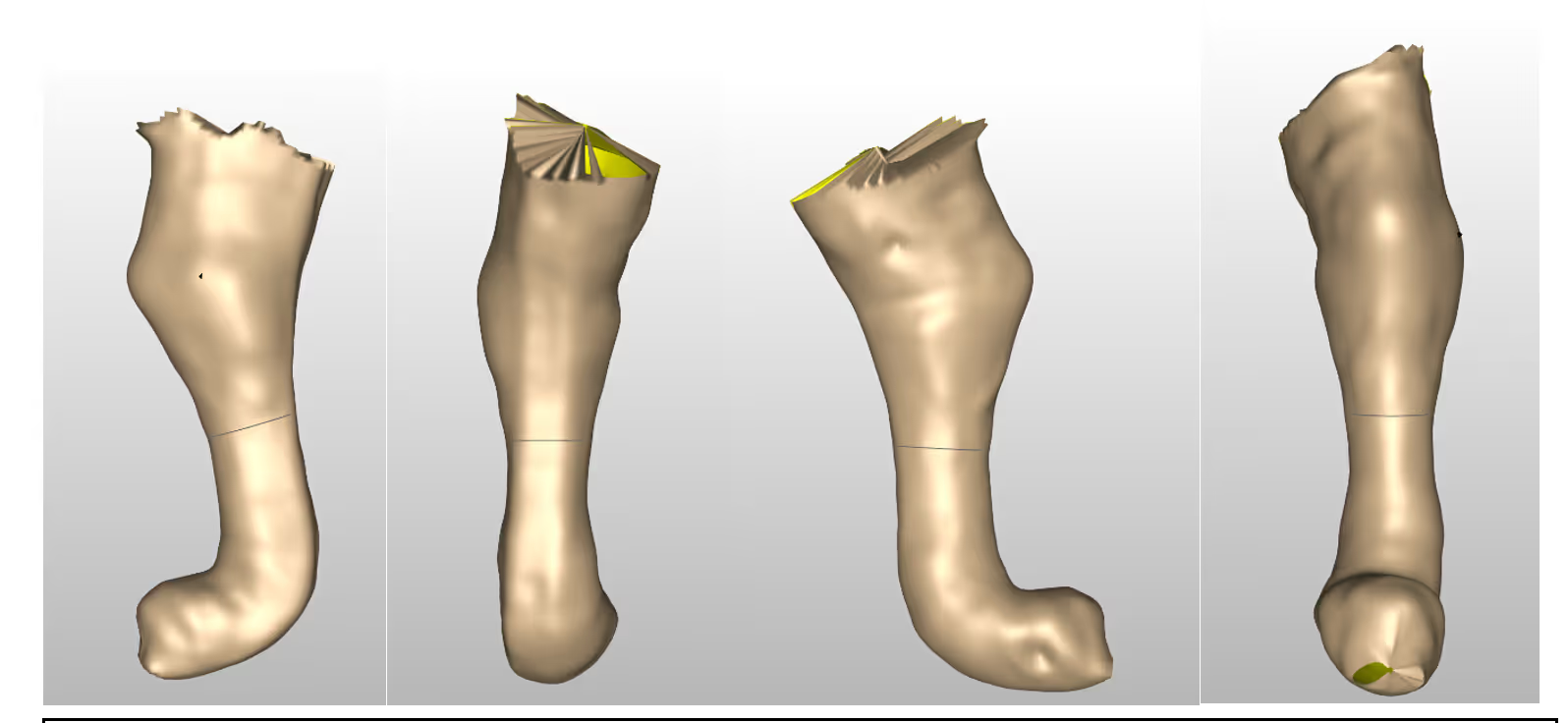
POP is calcinated gypsum. When the plaster roll is dipped in water, and wrapped around an affected limb, an exothermic reaction is created, and the plaster slowly turns from a malleable roll of fabric-like tape to a solid state within a matter of minutes.
While POP is now rarely used in human medicine for casting and immobilization, it is used regularly in human orthotics and prosthetics to obtain an accurate impression of the affected limb.
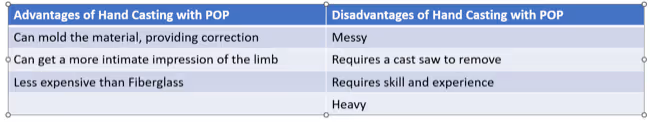
Advantages of hand casting with POP include: the ability to mold the material, provide correction of the limb, obtaining a more intimate impression of the limb and it’s less expensive than Fiberglass. Disadvantages of hand casting with POP include: POP is quite messy, requires a cast saw to remove, requires human skill and experience, and the material is heavy when used for bandaging and immobilization purposes.
Fiberglass replaces POP for casting and immobilization
Fiberglass, is a fiber reinforced polymer made from a plastic matrix reinforced by fine glass, and functions as a newer, synthetic alternative to POP2. Fiberglass was first used in human medicine during the 1970s as the fiberglass material was much lighter (1/3 the weight of POP), more durable (three times stronger than POP), much cleaner to work with, yielded less skin complications and was ultimately more comfortable for the patient2. Today, in human orthotics, fiberglass is commonly used to obtain an accurate impression of the affected limb. Many seasoned CPOs may argue that POP does a better job of obtaining an accurate impression of the residual limb in human prosthetics.
The veterinary field embraced fiberglass in the 1980s, again replacing POP, for casting and immobilization purposes. Wound complications are common when using fiberglass for casting and immobilization of an animal’s limb. We won’t get into that here – that is an entirely different blog post!
Advantages to hand casting with fiberglass include: the ability to mold the material, provide a correction to the limb, obtain an intimate impression of the limb, less mess is created, the material is 1/3 the weight of POP when used for bandaging and immobilization purposes and in animals, the hair and fur coat are contained. Disadvantages of hand casting with fiberglass include: a slightly less intimate impression when compared to POP, requires human skill and experience, and it’s more expensive than POP.

The advent of digital limb capture
Digital limb capture, in the form of scanning the affected limb with a three-dimensional (3D) laser scanner, was implemented in the human O&P world in 2011. A main benefit of this application with humans when compared to animals, is that the human can listen and can rationalize instructions, for example when a CPO gives a patient instruction to sit still and hold a certain position for the duration of the scan.
To date while the human O&P literature comparing the speed, accuracy, and reliability of 3D scanning with traditional methods of casting is limited, the speed of scanning (a human) is fast in the hands of a skilled clinician, the accuracy and reliability between 3D scanning and traditional methods of casting remains variable3. Translation? The human O&P jury is still out, determining how scanning versus casted impressions compare.
In the veterinary O&P world, our patients do not listen, nor can they rationalize; thus, scanning the live animal’s limb in real time brings a unique set of challenges, and would most definitely not be faster than casting a fiberglass impression.
The perceived disadvantages of digital limb capture outweigh any brainstormed advantage: There is a financial investment required to obtain the equipment, and a steep learning curve for the clinician for sure. More importantly, the limb cannot be touched while scanning, thus no correction can be applied to the limb, the scan does not provide an intimate impression of the limb (again since nothing is touching the limb), the hair and fur-coat are uncontained, which can lead to variability of data collected, and most importantly, the animal is awake, which can lead to motion causing the scan to have to start over and the animal is restrained and held in an unnatural stance position, which can affect the joint angles of the alignment of the limb. Thus, with digital limb capture of a live animal’s affected limb, the data collected can misrepresent the clinical presentation entirely.
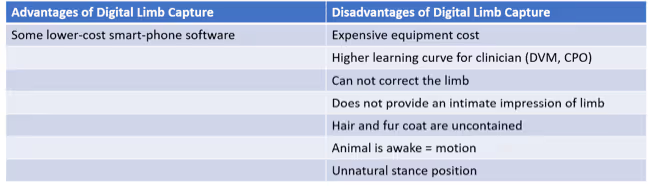
As of late, there are several lower-cost, smartphone-based scanning software systems available. However, there is little scientific evidence indicating the accuracy or reliability of these lower-cost scanning alternatives4.
What makes Hand Casting in Animals Successful?
In the twenty years that OrthoPets has been treating animals of all sizes with orthotic and prosthetic devices, we have learned the following clinical pearls that greatly increase the success of hand casting:
1. The utilization of a skilled DVM or CPO who hand casts the impression.
2. The utilization of a skilled and credentialed veterinary technician for restraint of the animal.
3. The use of sedation if needed and if able to be tolerated by the animal.
4. The recumbency of the animal matters:
o Stifle Orthosis – the animal is positioned standing, as this allows for normal joint angles (alignment) and weightbearing during hand casting.
o All other devices (Carpal Orthosis, Tarsal Orthosis, Prosthesis or Prosthosis) – the animal is positioned in lateral recumbency, so that correction and proper alignment can be applied to the affected limb during hand casting.
Bobbie Adams is the CEO and owner of Pawsthetics and works for OrthoPets, connecting CPO's with Veterinarians. Bobbie is the only provider of orthotics and prosthetics for animals, who is both a Registered Veterinary Technician (RVT) and a Licensed Prosthetist Orthotist (LPO) in the state of Oklahoma, maybe even in the country. www.pawsthetics.com
References
1. Sharma H, Prabu D. Plaster of Paris: Past, present and future. J Clin Orthop Trauma. 2013 Sep;4(3):107-9. doi: 10.1016/j.jcot.2013.09.004. PMID: 26403547; PMCID: PMC3880430.
2. Szostakowski B, Smitham P, Khan WS. Plaster of Paris-Short History of Casting and Injured Limb Immobilzation. Open Orthop J. 2017 Apr 17;11:291-296. doi: 10.2174/1874325001711010291. PMID: 28567158; PMCID: PMC5420179.
3. Farhan M, Wang JZ, Bray P, Burns J, Cheng TL. Comparison of 3D scanning versus traditional methods of capturing foot and ankle morphology for the fabrication of orthoses: a systematic review. J Foot Ankle Res. 2021 Jan 7;14(1):2. doi: 10.1186/s13047-020-00442-8. PMID: 33413570; PMCID: PMC7792297.
4. Dickinson, Alexander S. PhD; Donovan-Hall, Maggie K. PhD; Kheng, Sisary MSc; Bou, Ky DPO (ISPO Cat II); Tech, Auntouch DPO (ISPO Cat II); Steer, Joshua W. PhD; Metcalf, Cheryl D. PhD; Worsley, Peter R. PhD. Selecting Appropriate 3D Scanning Technologies for Prosthetic Socket Design and Transtibial Residual Limb Shape Characterization. Journal of Prosthetics and Orthotics 34(1):p 33-43, January 2022. | DOI: 10.1097/JPO.0000000000000350